Pain Management
The Florida Division of Workers Compensation this month published a notice in the Florida Administrative Register announcing plans to review physician dispensing rules.

Teva Pharmaceutical Industries Ltd. and AbbVie Inc.s Allergan unit on Tuesday reached a $58 million settlement with the city of San Francisco just before completion of a trial over claims that they fueled an opioid epidemic in the city.

Texas Attorney General Ken Paxton said on Tuesday he was investigating whether Walmart improperly filled prescriptions and failed to report suspicious orders when selling opioid drugs.
The Delaware Supreme Court on Thursday upheld a determination that an injured workers prescribed narcotic pain medications were no longer compensable.
The U.S. Supreme Court on Monday gave two doctors found guilty of misusing their licenses in the midst of the U.S. opioid epidemic to write thousands of prescriptions for addictive pain medications another chance to challenge their convictions.
Payments for dermatological agents continue to increase while payments for opioids continue to decline, according to a report released Thursday by the Workers Compensation Research Institute.

The average medical cost-per-claim for injured workers with lower back pain who were treated exclusively by a chiropractor was 61% less than for those who received no chiropractic treatment, according to a new report.

A group of Florida workers compensation insurers is challenging the legitimacy of a state policy they claim improperly requires them to authorize physicians and other providers to dispense medications to injured workers.
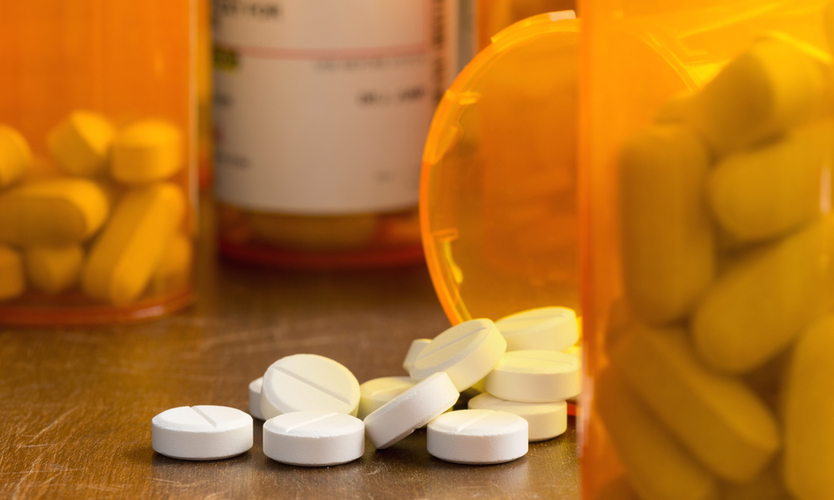
Despite substantial reductions in recent years, opioids continue to be widely dispensed to workers with work-related injuries in several states, according to a study released Thursday by the Workers Compensation Research Institute.
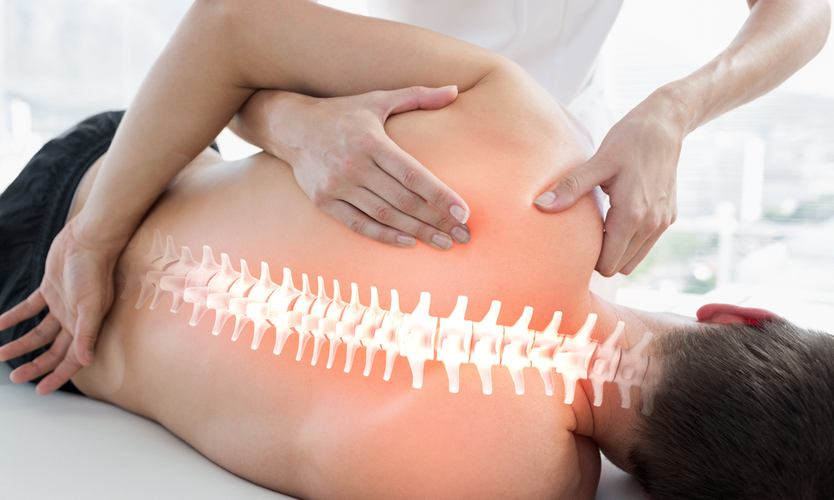
Ford Motor Co. does not have to cover massage therapy for an injured worker in part because the treatment was not prescribed by a doctor, an appeals court in Michigan ruled Thursday.

Musculoskeletal disorders can be treated more effectively by medications and therapies other than opioids, according to new research that shows injuries that make up the lions share of workers compensation claims can avoid dangerous drug remedies.
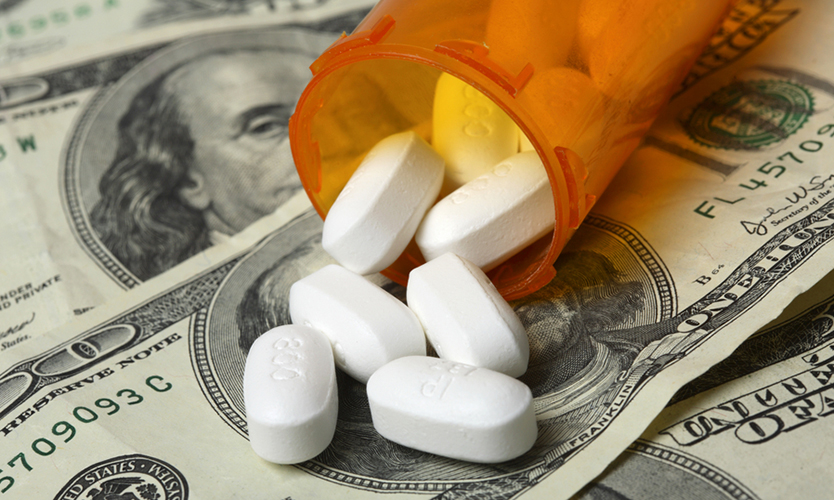
Workers compensation pharmacy spending decreased 6.1% in 2019, a decline attributed to a number of factors including fewer opioids, more generic drugs, and lower costs via home delivery, according to new data released Wednesday by Matrix Healthcare Services Inc., a Tampa, Florida-based pharmacy benefits manager doing business as myMatrixx.

The National Council of Insurance Legislators voted to adopt a workers compensation drug formulary model, the council announced Wednesday.

A study released earlier this month showed a 6.7% decline in workers compensation claim activity where states have approved medical marijuana.
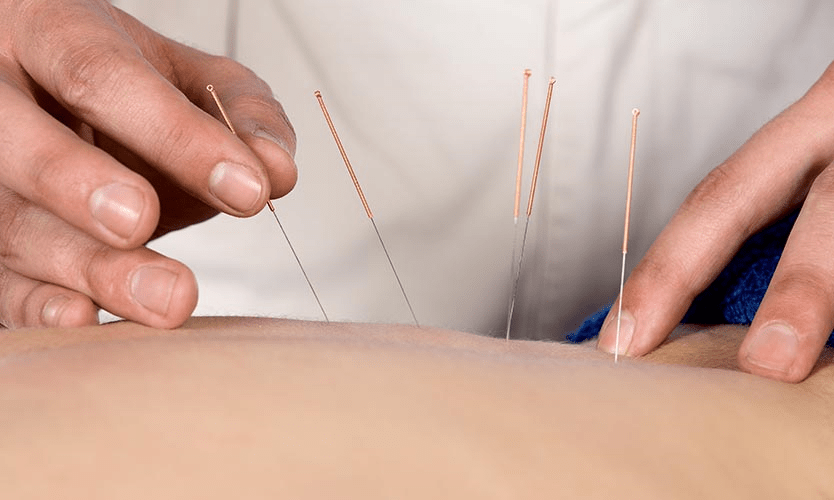
Opioid dispensing in workers compensation continues to be a hot issue as experts see the number of prescriptions continue to decrease in favor of physical medicine, non-opioid medications and behavioral interventions to treat pain.

A Louisiana lawmaker is pushing for the state to adopt a resolution creating a pilot program to address opioid abuse among those seeking lower-back pain care management.

A Louisiana lawmaker is pushing for the state to adopt a resolution creating a pilot program to address opioid abuse among those seeking lower-back pain care management.
Opioid dispensing in workers compensation continues to be a hot issue as experts see the number of prescriptions continue to decrease in favor of physical medicine, non-opioid medications and behavioral interventions to treat pain.

A study released earlier this month showed a 6.7% decline in workers compensation claim activity where states have approved medical marijuana.

The National Council of Insurance Legislators voted to adopt a workers compensation drug formulary model, the council announced Wednesday.

An employer may be required to reimburse a pharmacy for a nearly $5,000 compound cream prescribed to a worker for his shoulder injury because it failed to seek utilization review.

Beginning Thursday, doctors in New York who need to prescribe drugs to injured workers will be required to adhere to the state’s drug formulary, a new system that classifies drugs as appropriate or requiring preauthorization, and includes an online portal to preauthorize certain medications such as opioids.

Eighty-one percent of primary care physicians surveyed recently said they are reluctant to take on patients who are on opioids, according to findings released in October by Quest Diagnostics Inc.


